Hidden Signs Your Gut Is Inflamed (That Have Nothing to Do With Digestion)
Mar 17, 2026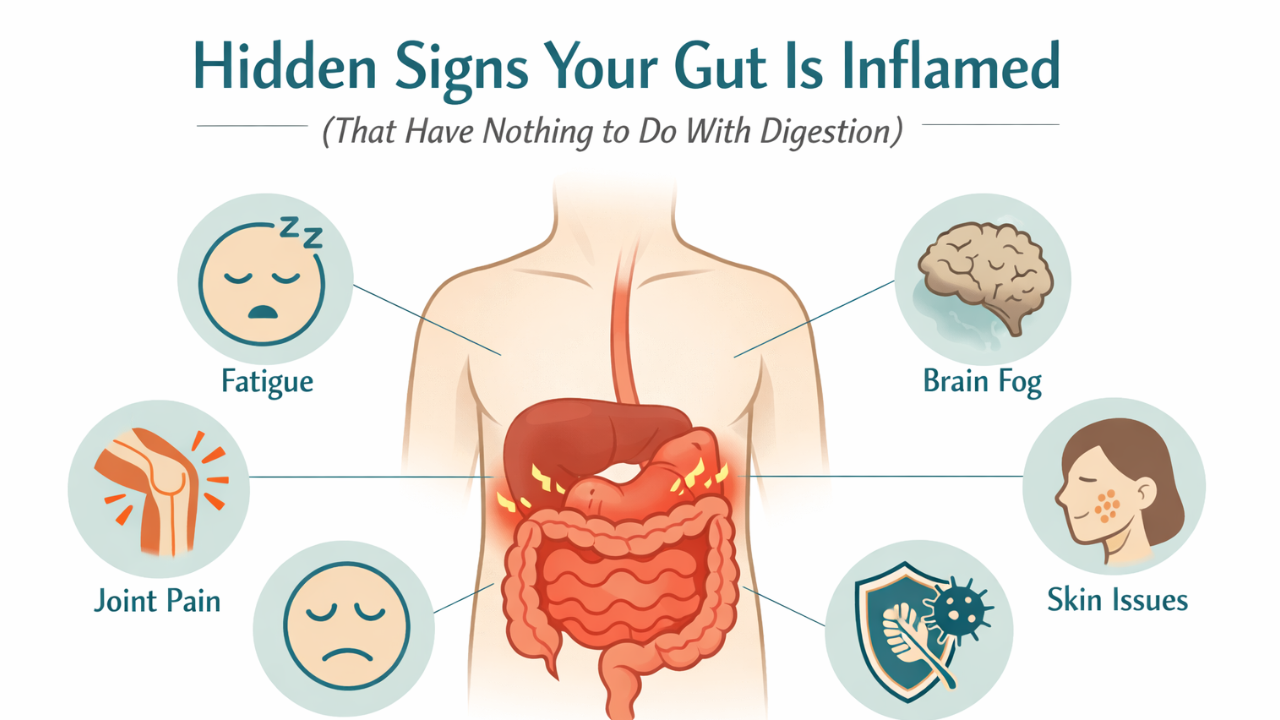
When people think about gut problems they usually imagine symptoms like bloating, diarrhea, reflux, or stomach pain. While those can certainly occur, gut inflammation often shows up in ways that seem completely unrelated to digestion. In fact, many people with significant gut dysfunction have very few digestive complaints at all.
When I refer to the gut, I don’t mean the digestive system. It technically is bacteria flora. It is deeply connected to the immune system, the brain, hormones, and even the musculoskeletal system. Roughly seventy percent of the immune system lives in the gut, and the intestinal lining acts as a barrier that carefully regulates what enters the bloodstream. When that lining becomes inflamed or disrupted, it can trigger widespread effects throughout the body.
Because of this, gut inflammation can show up in surprising ways.
One of the most common signs is chronic fatigue. When the gut barrier is compromised, bacterial fragments and inflammatory compounds can enter circulation. The immune system responds by activating inflammatory pathways, which can leave people feeling constantly tired or drained. This type of fatigue often does not improve with more sleep because it is driven by immune activation rather than simple rest deprivation.
Brain fog is another frequent clue. The gut and brain communicate through the gut brain axis, a network that includes the vagus nerve, immune signals, and microbial metabolites. When gut inflammation is present, inflammatory cytokines can influence brain function. Many people notice difficulty concentrating, slower thinking, or a feeling that their mind is not as sharp as it used to be.
Skin issues are also strongly connected to gut health. Conditions like eczema, acne, rosacea, and psoriasis often worsen when the gut microbiome becomes imbalanced. The immune system may react to microbial byproducts entering circulation, leading to inflammation that manifests through the skin. In some individuals, improving gut health can significantly calm persistent skin conditions.
Joint pain is another hidden sign that often surprises people. When inflammatory compounds circulate in the body they can affect connective tissues and joints. This is one reason individuals with gut dysfunction sometimes experience unexplained aches or stiffness. Inflammatory mediators produced in the gut can contribute to systemic inflammation that aggravates joints and tendons.
Mood changes are another overlooked connection. The gut microbiome plays a major role in producing neurotransmitters and regulating stress responses. Inflammation in the gut can disrupt these pathways and influence mood. Anxiety, irritability, and low mood can sometimes be tied to gut dysfunction even when digestion feels relatively normal.
Food sensitivities are also a common indicator of gut inflammation. When the intestinal barrier becomes more permeable, larger food particles can cross into circulation where the immune system recognizes them as foreign. This can lead to immune reactions that cause fatigue, headaches, skin reactions, or joint pain after eating certain foods.
Frequent illnesses can also be a clue. Because the gut houses a large portion of the immune system, chronic gut inflammation can weaken immune resilience. People may find themselves catching colds more easily or taking longer to recover from infections.
Understanding these connections highlights why gut health is central to overall wellness. When the gut becomes inflamed, the effects are rarely limited to digestion alone. The immune system, brain, skin, joints, and metabolism can all be influenced by what is happening in the intestinal environment.
Supporting gut health often involves several key strategies. Reducing highly processed foods, excess sugar, and inflammatory oils can help calm immune activation. Increasing fiber rich foods supports beneficial gut bacteria that produce anti inflammatory compounds. Managing stress is also important because chronic stress can directly disrupt the gut barrier and microbiome.
In some cases targeted approaches such as improving microbial balance, addressing infections, or repairing the intestinal lining may be necessary. Functional medicine practitioners often look deeper into these underlying contributors rather than focusing only on surface symptoms.
The takeaway is that gut inflammation rarely stays confined to the gut. When unexplained symptoms appear in the brain, skin, joints, or immune system, it may be worth looking deeper at the health of the digestive system.
The gut often speaks through signals that do not look like digestion at all.
